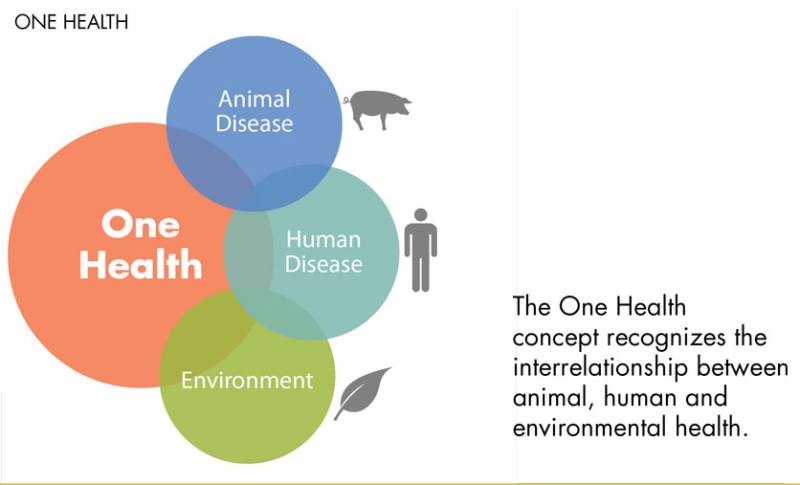
Dr Sayema Awais writes that newly emerging infections such as COVID-19 cannot be handled without adopting a 'one health' approach that calls for seeking synergy between health of humans, animals and their shared environment.
Why do people wonder that the current COVID-19 pandemic has been brought about by a conspiracy? Why do they wonder if an unseen hand has been at play to create a pathogen leading to the unbridled devastation caused by the Coronavirus? Those who predicted this pandemic are being accused of having concocted the plan to mint money at the expense of millions of human lives. If you look closely, the ingredients required for the emergence of an infectious disease of this proportion have been brewing since long.
Human population has been growing at an exponential rate for the past century or so, thanks to the control of infectious diseases and the advancement of medical sciences leading to improved survival rates and longevity. This increase in life span paved the way for a change in the age structure of populations and the emergence of an older population with higher morbidity and greater vulnerability.
Another consequence of the population growth was the penetration of previously uninhabited regions of the world. In the process, humans have been increasingly exposed to new sources of infectious agents. Massive deforestation, unrestrained urbanization and overpopulation combined with breakdown of sanitation has led to circumstances where people are often living in close proximity with domestic animals – conditions conducive to the appearance of zoonotic diseases – diseases that are transmitted from animals to humans.
As the consumption of meat and meat products gradually increased worldwide to unprecedented levels, the use of drugs to increase the weight of animals and the use of antibiotics to control infections among animals bred under unhygienic and restricted environments have become commonplace with complete disregard to the consequences such as, increasing antimicrobial resistance. With greater economic development and affluence, travel and transport of goods has become swifter also facilitating the spread of infectious agents. In response to an increasing indulgence in exotic foods, “wet markets” have sprung up to cater to the insatiable desires of the rich. The close proximity of humans and animals kept under cramped, filthy environs until they are slaughtered to be sold creates the kind of conditions that lead to spillover of infections with the potential to reach distant lands carried by unsuspecting customers visiting from another continent. These wet markets served as breeding grounds for the emergence of the infectious H1N1 Coronavirus which caused Severe Acute Respiratory Syndrome (SARS) in 2009. The circumstances that led to the COVID 19 pandemic were not so different either.
Such emerging infections, however, are not new developments. There are many examples where the causative organism crossed the boundary from one species to another, including Human Immunodeficiency Virus (HIV) which probably emerged from the Simian Immunodeficiency Virus found in non-human primates and the Creutzfeldt-Jacob Disease thought to have originated from the Bovine Spongiform Encephalopathy (BSE)/ mad cow disease. MERS or Middle Eastern Respiratory Syndrome – an infection that originated in bats and transmitted through camels to humans was one of the recent ones that emerged in 2003.
The emergence of such infections is, therefore, not an event that could not have been predicted. Right now when we are planning to prevent the spread of COVID-19 infection and scientists all over the world are scrambling to produce an effective vaccine, we also need to pay heed to the underlying factors which led to the emergence of this pandemic. This is because real prevention is to control the source of infection. And such infections are still likely to emerge in the not so distant future.
The World Health Organization has long advocated the concept of “One Health Approach” urging governments to pay attention to the complex interactions between humans, animals, plant life, and the environment that we all share. “One Health” refers to the fact that health of humans is connected to the health of animals and their shared environment. Communications between human health professionals (doctors, nurses, public health professionals & epidemiologists) and veterinary professionals (veterinarians, agricultural experts), environmentalists and other experts should be facilitated to identify critical issues at the human-environment-animal interface that can be tackled by a coordinated effort. Other important players in this effort can be law makers, farmers, communities, and industrialists.
Changes in the climate brought about by the fuel intensive airline industry, use of fertilizers, insecticides, pesticides and hormone-containing animal feed in agriculture, release of toxic by-products into the sewerage system by chemical industries – each of these events can trigger chains of events adversely affecting plant, animal and human life. The “One Health” approach allows us to recognize the deviant behaviours of humans wreaking havoc on the natural ecosystems and damaging both animal and human life through irresponsibility and neglect. If we continue to try and carry out “business as usual”, such pandemics are likely to become the “usual” occurrence and a not a “once in a lifetime” phenomenon. Governments should pay heed to the preservation of natural ecosystems, protecting wildlife and combating pollution and destruction of natural habitats.
In Pakistan, there is little, if any, coordinated interaction between public health professionals, veterinarians, environmentalists and agriculture experts. A new platform should be created to bring together the leading professionals in these fields with a plan to keep an eye on new emerging diseases at home and abroad. Capacity building initiatives should be introduced to allow professionals to engage with new local research while maintaining communication and collaboration with international research bodies. Developing a national surveillance system at the intersection of the various disciplines will shorten the response time to threats of epidemics and improve emergency preparedness. New developments in diagnostics and therapeutics, in human as well as veterinary medicine, should be tested and replicated at national level to improve the ability to investigate and control epidemics.
Why do people wonder that the current COVID-19 pandemic has been brought about by a conspiracy? Why do they wonder if an unseen hand has been at play to create a pathogen leading to the unbridled devastation caused by the Coronavirus? Those who predicted this pandemic are being accused of having concocted the plan to mint money at the expense of millions of human lives. If you look closely, the ingredients required for the emergence of an infectious disease of this proportion have been brewing since long.
Human population has been growing at an exponential rate for the past century or so, thanks to the control of infectious diseases and the advancement of medical sciences leading to improved survival rates and longevity. This increase in life span paved the way for a change in the age structure of populations and the emergence of an older population with higher morbidity and greater vulnerability.
Another consequence of the population growth was the penetration of previously uninhabited regions of the world. In the process, humans have been increasingly exposed to new sources of infectious agents. Massive deforestation, unrestrained urbanization and overpopulation combined with breakdown of sanitation has led to circumstances where people are often living in close proximity with domestic animals – conditions conducive to the appearance of zoonotic diseases – diseases that are transmitted from animals to humans.
As the consumption of meat and meat products gradually increased worldwide to unprecedented levels, the use of drugs to increase the weight of animals and the use of antibiotics to control infections among animals bred under unhygienic and restricted environments have become commonplace with complete disregard to the consequences such as, increasing antimicrobial resistance. With greater economic development and affluence, travel and transport of goods has become swifter also facilitating the spread of infectious agents. In response to an increasing indulgence in exotic foods, “wet markets” have sprung up to cater to the insatiable desires of the rich. The close proximity of humans and animals kept under cramped, filthy environs until they are slaughtered to be sold creates the kind of conditions that lead to spillover of infections with the potential to reach distant lands carried by unsuspecting customers visiting from another continent. These wet markets served as breeding grounds for the emergence of the infectious H1N1 Coronavirus which caused Severe Acute Respiratory Syndrome (SARS) in 2009. The circumstances that led to the COVID 19 pandemic were not so different either.
Such emerging infections, however, are not new developments. There are many examples where the causative organism crossed the boundary from one species to another, including Human Immunodeficiency Virus (HIV) which probably emerged from the Simian Immunodeficiency Virus found in non-human primates and the Creutzfeldt-Jacob Disease thought to have originated from the Bovine Spongiform Encephalopathy (BSE)/ mad cow disease. MERS or Middle Eastern Respiratory Syndrome – an infection that originated in bats and transmitted through camels to humans was one of the recent ones that emerged in 2003.
The emergence of such infections is, therefore, not an event that could not have been predicted. Right now when we are planning to prevent the spread of COVID-19 infection and scientists all over the world are scrambling to produce an effective vaccine, we also need to pay heed to the underlying factors which led to the emergence of this pandemic. This is because real prevention is to control the source of infection. And such infections are still likely to emerge in the not so distant future.
The World Health Organization has long advocated the concept of “One Health Approach” urging governments to pay attention to the complex interactions between humans, animals, plant life, and the environment that we all share. “One Health” refers to the fact that health of humans is connected to the health of animals and their shared environment. Communications between human health professionals (doctors, nurses, public health professionals & epidemiologists) and veterinary professionals (veterinarians, agricultural experts), environmentalists and other experts should be facilitated to identify critical issues at the human-environment-animal interface that can be tackled by a coordinated effort. Other important players in this effort can be law makers, farmers, communities, and industrialists.
Changes in the climate brought about by the fuel intensive airline industry, use of fertilizers, insecticides, pesticides and hormone-containing animal feed in agriculture, release of toxic by-products into the sewerage system by chemical industries – each of these events can trigger chains of events adversely affecting plant, animal and human life. The “One Health” approach allows us to recognize the deviant behaviours of humans wreaking havoc on the natural ecosystems and damaging both animal and human life through irresponsibility and neglect. If we continue to try and carry out “business as usual”, such pandemics are likely to become the “usual” occurrence and a not a “once in a lifetime” phenomenon. Governments should pay heed to the preservation of natural ecosystems, protecting wildlife and combating pollution and destruction of natural habitats.
In Pakistan, there is little, if any, coordinated interaction between public health professionals, veterinarians, environmentalists and agriculture experts. A new platform should be created to bring together the leading professionals in these fields with a plan to keep an eye on new emerging diseases at home and abroad. Capacity building initiatives should be introduced to allow professionals to engage with new local research while maintaining communication and collaboration with international research bodies. Developing a national surveillance system at the intersection of the various disciplines will shorten the response time to threats of epidemics and improve emergency preparedness. New developments in diagnostics and therapeutics, in human as well as veterinary medicine, should be tested and replicated at national level to improve the ability to investigate and control epidemics.
